
VP for Research
Old lungs are not as capable as young lungs of fighting off an infection of the bacteria that causes tuberculosis (TB), placing seniors at a greater risk of developing TB. The microbe that causes this infectious disease, Mycobacterium tuberculosis (Mtb), currently kills more people in the world than any other pathogen.
“Things go wrong as we get older,” said Professor Joanne Turner, Ph.D., Vice President for Research. “When we’re younger, we have control mechanisms in place, and our body will switch on responses and switch off responses as needed. As we get older, some of those responses become defective.”
Texas Biomed researchers published an article in the Journal of Infectious Diseases in July 2019. The study details an experiment that took place in vitro (in the lab) and in vivo (in animals) that showed fluid in the lining of the lungs plays a big role in the elderly’s susceptibility to infection with the bacterium Mtb.
The team studied the role of the lung mucosa (a.k.a., alveolar lining fluid), which is the layer of liquid in the lungs that assists in gas exchange and also plays a protective role against infection. Those samples were acquired from volunteers who underwent a bronchoalveolar lavage, a medical procedure in which a bronchoscope is passed through the mouth or nose into the lungs and fluid is squirted into a small part of the lung and then collected for examination. Half of the donor volunteers were from San Antonio; the other half were from Ohio. In San Antonio, Texas Biomed researchers are collaborating with the Pulmonary and Critical Care Medicine Division at UT Health San Antonio, Drs. Jay Peters and Diego Maselli Caceres.
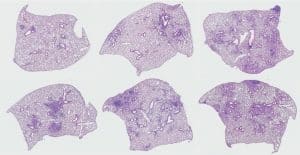
Researchers incubated Mtb with this fluid at its physiological concentrations within the human lung. In healthy, young donors, the molecules in the lung lining fluid would interact with Mtb send bacteria to macrophages (immune cells) to be killed. However, in older donors, the molecules in the lung lining fluid present some dysfunctionalities, allowing bacteria to infect and grow within macrophages, thus driving susceptibility and higher risk of infection.
When the same experiment was conducted in vivo in healthy young mice, results recapitulated what happened in the in vitro experiment. The animals that received Mtb that had been incubated in lung lining fluid from older humans could not control the infection as well as animals that received Mtb incubated with lung lining fluid from a younger person.
“We hypothesized that the status of the lung mucosa may partially explain why we are susceptible to respiratory infectious diseases as we age,” explained Professor Jordi Torrelles, Ph.D., Co-lead of the Population Health program at Texas Biomed. “Elderly individuals (65 and older) have higher degree of oxidation in their lung mucosa. In our study we demonstrated that this oxidation alters the normal function of important lung mucosa innate soluble components involved in the control of infectious agents reaching our lungs. With this control impaired as we age, we are more susceptible to respiratory infections. We are currently collaborating with Southwest Research Institute investigators (Dr. Hong Dixon and Varsin Archer) to establish if reversal of the oxidative status of the lung mucosa in the elderly could make us resistant to respiratory infections.”
Scientists will be looking at ways to intervene in this process to make these molecules in the lungs of elderly people more functional.

Population Health Co-lead
“The most exciting thing this study tells us is that the very first interaction between a pathogen and the fluid in the lung can dictate long term outcome,” Dr. Turner said. “You could perform lots of interventions throughout the entire infection period. But if you change that first interaction, you could potentially dictate whether that person develops active TB, controls it better or even clears it.”
Other Texas Biomed researchers who authored the paper include Larry Schlesinger, M.D., Juan Moliva, Ph.D., Angélica Olmo-Fontánez, Maria Montoya, Abul Azad, Ph.D., Russell Ault, Julia Scordo, Ph.D., Eusondia Arnett, Ph.D., and Anwari Akhter.
Funding for this project came from the National Institute on Aging (NIA), NIH (grant number P01 AG-051428, the National Institute of General Medical Sciences at NIH (grant number T32 GM068412, the National Institute of Allergy and Infectious Diseases of the NIH (grant number R01 AI93570-S1), and a supplement by the NIA (grant number P01 AG-051428-S1). Dr. Torrelles’ work is also supported by the Robert J. Kleberg, Jr., and Helen C. Kleberg Foundation.