
Malaria is worldwide scourge infecting 200 million people around the world and killing more than 400,000 of them. The parasite is carried by the Anopheles mosquito, particularly in tropical areas like Sub-Saharan Africa and Asia.
Texas Biomed scientists are “particularly interested in the evolution of drug resistance,” said Scientist Tim Anderson, Ph.D., adding that it is “a recurring problem in controlling tropical diseases.”
Artemisinin is a recently discovered drug that is the gold standard for treating malaria, considered instrumental in reducing the number of cases of the infectious disease over the last decade. However, more than 125 mutation variations of drug resistance have emerged in Southeast Asia. Those mutations impact the metabolism of the parasite itself – inhibiting growth rate, for instance.
A recent NIH-funded study published in the journal Antimicrobial Agents and Chemotherapy by Anderson and his team looked at one particular drug resistant variant sequence (called an allele) that is outpacing the others. Anderson’s team wanted to test the idea that successful resistance alleles have fewer adverse consequences for the parasites and, thus, thrived and spread.

Senior Research Associate Shalini Nair, who has worked at Texas Biomed for 18 years, was a key part of this project. “I started out by figuring out how to use CRISPR-Cas9 to edit key mutations in the malaria parasite,” Nair explained. CRISPR is short for clustered regularly interspaced short palindromic repeats. It’s a system for genome editing, using the cell’s own DNA repair mechanism to add or delete pieces of genetic material.
To maximize the relevance of their results, the team used “a recently isolated parasite clone from the Thailand-Myanmar border for manipulation rather than a laboratory adapted parasite clone,” the journal article stated.
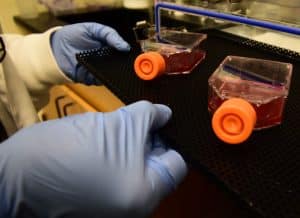
In a head-to-head comparison between two mutants – one strong and thriving in patients and one not as strong and waning – researchers grew the parasites in flasks of blood cells in the lab. Scientists measure how the mutations impacted the “fitness” of the parasites. In other words, they checked to see if the mutations impacted the metabolism of the more common and less common strains in the expected way. Scientists hypothesized the more common and thriving mutations would have less “fitness cost” to the parasite.
The cultures were maintained for 60 days. Then they extracted DNA and amplified it, comparing frequencies of the different mutations.
Xue Li, Ph.D., is a post-doctoral student who compiled the data from the study. “Our results were not the same as our hypothesis,” Li stated. The scientists want to see if there are other mutations in different areas of the genome impacting whether these drug-resistant parasites flourish or fail. The answer may be more complicated than first thought.
Dr. Anderson emphasized that malaria researchers like his team need to understand the process by which parasites adapt to anti-malarials.” If we understand that,” he said, “we are in a far better position to then to develop more effective, evolution proof interventions.”